|
There is a lot of misinformation circling around in mainstream nutrition. I have listed the worst examples in this article, but unfortunately this is just the tip of the iceberg.
Here are the top 11 biggest lies, myths and misconceptions of mainstream nutrition. 1. Eggs Are Unhealthy There’s one thing that nutrition professionals have had remarkable success with… and that is demonizing incredibly healthy foods. The worst example of that is eggs, which happen to contain a large amount of cholesterol and were therefore considered to increase the risk of heart disease. But recently it has been proven that the cholesterol in the diet doesn’t really raise the cholesterol in blood. In fact, eggs primarily raise the “good” cholesterol and are NOT associated with increased risk of heart disease (1, 2). What we’re left with is one of the most nutritious foods on the planet. They’re high in all sorts of nutrients along with unique antioxidants that protect our eyes (3). To top it all of, despite being a “high fat” food, eating eggs for breakfast is proven to cause significant weight loss compared to bagels for breakfast (4, 5). Bottom Line: Eggs do not cause heart disease and are among the most nutritious foods on the planet. Eggs for breakfast can help you lose weight. 2. Saturated Fat is Bad For You A few decades ago it was decided that the epidemic of heart disease was caused by eating too much fat, in particular saturated fat. This was based on highly flawed studies and political decisions that have now been proven to be completely wrong. A massive review article published in 2010 looked at 21 prospective epidemiological studies with a total of 347,747 subjects. Their results: absolutely no association between saturated fat and heart disease (6). The idea that saturated fat raised the risk of heart disease was an unproven theory that somehow became conventional wisdom (7). Eating saturated fat raises the amount of HDL (the “good”) cholesterol in the blood and changes the LDL from small, dense LDL (very bad) to Large LDL, which is benign (8, 9). Meat, coconut oil, cheese, butter… there is absolutely no reason to fear these foods. Bottom Line: Newer studies have proven that saturated fat does not cause heart disease. Natural foods that are high in saturated fat are good for you. 3. Everybody Should be Eating Grains The idea that humans should be basing their diets on grains has never made sense to me. The agricultural revolution happened fairly recently in human evolutionary history and our genes haven’t changed that much. Grains are fairly low in nutrients compared to other real foods like vegetables. They are also rich in a substance called phytic acid which binds essential minerals in the intestine and prevents them from being absorbed (10). The most common grain in the western diet, by far, is wheat… and wheat can cause a host of health problems, both minor and serious. Modern wheat contains a large amount of a protein called gluten, but there is evidence that a significant portion of the population may be sensitive to it (11, 12, 13). Eating gluten can damage the intestinal lining, cause pain, bloating, stool inconsistency and tiredness (14, 15). Gluten consumption has also been associated with schizophrenia and cerebellar ataxia, both serious disorders of the brain (16, 17). Bottom Line: Grains are relatively low in nutrients compared to other real foods like vegetables. The gluten grains in particular may lead to a variety of health problems. 4. Eating a Lot of Protein is Bad For Your Bones and Kidneys A high protein diet has been claimed to cause both osteoporosis and kidney disease. It is true that eating protein increases calcium excretion from the bones in the short term, but the long term studies actually show the opposite effect. In the long term, protein has a strong association with improved bone health and a lower risk of fracture (18, 19). Additionally, studies don’t show any association of high protein with kidney disease in otherwise healthy people (20, 21). In fact, two of the main risk factors for kidney failure are diabetes and high blood pressure. Eating a high protein diet improves both (22, 23). If anything, a high protein diet should be protective against osteoporosis and kidney failure! Bottom Line: Eating a high protein diet is associated with improved bone health and a lower risk of fracture. High protein also lowers blood pressure and improves diabetes symptoms, which should lower the risk of kidney failure. 5. Low-Fat Foods Are Good For You Do you know what regular food tastes like when all the fat has been taken out of it? Well, it tastes like cardboard. No one would want to eat it. The food manufacturers know this and therefore they add other things to compensate for the lack of fat. Usually these are sweeteners… sugar, high fructose corn syrup or artificial sweeteners like aspartame. We’ll get to the sugar in a moment, but I’d like to point out that even though artificial sweeteners don’t have calories, the evidence does NOT suggest that they are better for you than sugar. In fact, many observational studies show a consistent, highly significant association with various diseases like obesity, metabolic syndrome, diabetes, heart disease, premature delivery and depression (24, 25, 26). In these low-fat products, healthy natural fats are being replaced with substances that are extremely harmful. Bottom Line: Low-fat foods are usually highly processed products loaded with sugar, corn syrup or artificial sweeteners. They are extremely unhealthy. 6. You Should Eat Many Small Meals Throughout The Day The idea that you should eat many small meals throughout the day in order to “keep metabolism high” is a persistent myth that doesn’t make any sense. It is true that eating raises your metabolism slightly while you’re digesting the meal, but it’s the total amount of food that determines the energy used, NOT the number of meals. This has actually been put to the test and refuted multiple times. Controlled studies where one group eats many small meals and the other the same amount of food in fewer meals show that there is literally no difference between the two (27, 28). In fact, one study in obese men revealed that eating 6 meals per day led to less feelings of fullness compared to 3 meals (29). Not only is eating so often practically useless for most of the people out there, it may even be harmful. It is not natural for the human body to be constantly in the fed state. In nature, we used to fast from time to time and we didn’t eat nearly as often as we do today. When we don’t eat for a while, a cellular process called autophagy cleans waste products out of our cells (30). Fasting or not eating from time to time is good for you. Several observational studies show a drastically increased risk of colon cancer (4th most common cause of cancer death), numbers going as high as a 90% increase for those who eat 4 meals per day compared to 2 (31, 32, 33). Bottom Line: There is no evidence that eating many small meals throughout the day is better than fewer, bigger meals. Not eating from time to time is good for you. Increased meal frequency is associated with colon cancer. 7. Carbs Should Be Your Biggest Source of Calories The mainstream view is that everyone should eat a low-fat diet, with carbs being around 50-60% of total calories. This sort of diet contains a lot of grains and sugars, with very small amounts of fatty foods like meat and eggs. This type of diet may work well for some people, especially those who are naturally lean. But for those who are obese, have the metabolic syndrome or diabetes, this amount of carbohydrates is downright dangerous. This has actually been studied extensively. A low-fat, high-carb diet has been compared to a low-carb, high-fat diet in multiple randomized controlled trials. The results are consistently in favor of low-carb, high-fat diets (34, 35, 36). Bottom Line: The low-fat, high-carb diet is a miserable failure and has been proven repeatedly to be vastly inferior to lower-carb, higher-fat diets. 8. High Omega-6 Seed and Vegetable Oils Are Good For You Polyunsaturated fats are considered healthy because some studies show that they lower your risk of heart disease. But there are many types of polyunsaturated fats and they are not all the same. Most importantly, we have both Omega-3 fatty acids and Omega-6 fatty acids. Omega-3s are anti-inflammatory and lower your risk of many diseases related to inflammation (37). Humans actually need to get Omega-6s and Omega-3s in a certain ratio. If the ratio is too high in favor of Omega-6, it can cause problems (38). By far the biggest sources of Omega-6 in the modern diet are processed seed and vegetable oils like soybean, corn and sunflower oils. Throughout evolution, humans never had access to such an abundance of Omega-6 fats. It is unnatural for the human body. Research that specifically looks at Omega-6 fatty acids instead of polyunsaturated fats in general shows that they actually increase the risk of heart disease (39, 40). Eat your Omega-3s and consider supplementing with cod fish liver oil, but avoid the industrial seed and vegetable oils. Bottom Line: Humans need to get Omega-6 and Omega-3 fats in a certain ratio. Eating excess Omega-6 from seed oils raises your risk of disease. 9. Low Carb Diets Are Dangerous I personally believe low-carb diets to be a potential cure for many of the most common health problems in western nations. The low-fat diet peddled all around the world is fairly useless against many of these diseases. It simply does not work. However, low-carb diets (demonized by nutritionists and the media) have repeatedly been shown to lead to much better outcomes. Every randomized controlled trial on low-carb diets shows that they:
Bottom Line: Low-carb diets are the healthiest, easiest and most effective way to lose weight and reverse metabolic disease. It is a scientific fact. 10. Sugar is Unhealthy Because it Contains “Empty” Calories It is commonly believed that sugar is bad for you because it contains empty calories. It’s true, sugar has a lot of calories with no essential nutrients. But that is just the tip of the iceberg. Sugar, primarily because of its high fructose content, affects metabolism in a way that sets us up for rapid fat gain and metabolic disease. Fructose gets metabolized by the liver and turned into fat which is secreted into the blood as VLDL particles. This leads to elevated triglycerides and cholesterol (57, 58). It also causes resistance to the hormones insulin and leptin, which is a stepping stone towards obesity, metabolic syndrome and diabetes (59, 60). This is just to name a few. Sugar causes a relentless biochemical drive for humans to eat more and get fat. It is probably the single worst ingredient in the standard western diet. Bottom Line: The harmful effects of sugar go way beyond empty calories. Sugar wreaks havoc on our metabolism and sets us up for weight gain and many serious diseases. 11. High Fat Foods Will Make You Fat It seems kind of intuitive that eating fat would make you get fat.The stuff that is gathering under our skin and making us look soft and puffy is fat. So… eating fat should give our bodies even more of it. But it isn’t that simple. Despite fat having more calories per gram than carbohydrate or protein, high-fat diets do not make people fat. As with anything, this depends on the context. A diet that is high in fat AND high in carbs will make you fat, but it’s NOT because of the fat. In fact, diets that are high in fat (and low in carbs) cause much greater fat loss than diets that are low in fat (61, 62, 63). Source: https://authoritynutrition.com/11-biggest-lies-of-mainstream-nutrition/
0 Comments
 Here’s a sobering thought: advice doctors and dietitians give diabetics worldwide makes the condition life-threatening. University of Cape Town emeritus professor Dr Tim Noakes has set up The Noakes Foundation to do independent research into issues that include diabetes. Here, looks at why conventional medical and dietetic advice on diabetes is likely to be wrong. For starters, he shows why it has little if any science to back it up. Along the way, he shows why diabetes may turn out to be the most egregious example yet of iatrogenic (doctor-caused) disease. – Marika Sboros By Tim Noakes* My interest in the dietary management of diabetes stems from watching my father’s rapid downward physical decent in the years after he was diagnosed with Type 2 diabetes mellitus (T2DM); the diagnosis of T2DM in myself; and my reading of the “alternative” literature which convinces me that T2DM does not have to be an inevitably progressive disease: My conclusion is that unlike my father, it is not my pre-ordained fate to die from the final common pathway in fatal T2DM – disseminated obstructive arterial disease. But to achieve that I will have to ignore what I was taught and which, in turn, I have conveyed to two generations of students: So to prevent the development of the disseminated obstructive arterial disease of T2DM, I will have to follow dietary practices that are the polar opposite of those my father was advised to adopt and which hastened his death; advice that I personally practised for 33 years and which ultimately caused me also to develop T2DM. How could I have been so wrong? An article in the July 2016 issue of the magazine, Longevity, identifies the intellectual source of my errors. The article written by a “nutrition expert” seeks to explain why “foods that are minimally processed, such as starch that needs cooking, should provide most of the diabetic’s fuel for energy” (p. 44). The evidence is that “nutrients that increase the risk of diabetes are excess calories, high-GI/GL diets, animal fat and heme-iron (from meat). Nutrients that decrease the risk of developing diabetes are total fibre, cereal fibre, low GI/GL diets, plant-based foods, magnesium and vitamin D”. As a result food that are “out” for diabetics are “high protein intakes (more than 120-150g protein per day), red meat (unprocessed meat increases risk by 19% and processed meat by 51%), eggs (five to six eggs per day), white rice and sugar-sweetened beverages. Individual foods that decrease the diabetes risk are dairy, green leafy vegetables, whole grains (three portions per day), moderate alcohol and moderate coffee” (p 45). The problem with this advice is that it has no basis in hard science; it is a best guess based on studies that are too flawed to allow any firm conclusions. And certainly none good enough to tackle the one disease that poses the single greatest threat to the future of medicine as we currently understand it. To prove that each of these nutrients either causes or prevents T2DM would require at least 20 different 40-year studies in which we compared two groups of identical humans, all the members of the one group who eat the nutrient of interest in the correct amounts whilst all members of the other group do not. No other difference in any behaviour would be allowed between the 2 groups in our 20 separate studies. At the end of 40 years we would be able to determine which of those 20 nutrients, if any, either caused T2DM to be more or less prevalent in our tested groups. So to prove that, for example, 5 or 6 eggs a day causes T2DM whereas fewer than 5 does not (the inference from this statement), would require a 40 year study in which we compared two groups of identical humans, all the members of the one group ate “5 or 6” eggs a day, the other group’s members fewer than 5 eggs a day. Key is that the only allowed difference between the two groups must be the number of eggs eaten per day; nothing else may differ. We call this a randomized controlled trial (RCT). Ideally our RCT would require us to admit the two groups to jail to ensure that we can control everything in their lives (including how many eggs they each eat each day; how much exercise they do each day; whether or not they marry; how much they sleep each night etc etc etc). Unfortunately there is no other way to prove beyond a reasonable doubt that a single particular foodstuff is the direct and sole cause of a specific medical condition. Realizing that such studies are essentially impossible, influential US scientists directing research funding in the 1970s decided on a convenient scientific short cut. They agreed that, to save costs and allow the nutrition sciences to progress, they would in future accept findings from less rigorous research designs as valid “proof” of causation. So instead for the past 40 years, the nutrition sciences have been swamped by the cheaper alternative – observational (associational) studies (not experiments) that require only that specific populations be observed for decades as they go about their normal lives (without any experimental intervention). During their lives, the foods that each research subject eats is recorded on the assumption that this is an accurate measure of what each ate for the full duration of the study. Then the diseases that each participant develops during life are recorded with particular interest on when and why they died. The nutritional data are then analyzed to discover exactly which nutrients were eaten in excess by those who died from specific diseases. This method is based on one overriding assumption – that common diseases are caused by an excess intake of a single nutrient (with no other factor playing any role). As a result “proof” in this method is based on the circular argument shown below: But if this core assumption is untrue, the method will likely cause us to draw false conclusions. With potentially devastating consequences. But the real limitation of this experimental method is that, because it cannot exclude what we term “selection bias”, it can never prove that a single nutrient causes a specific disease. Selection bias means simply that the single nutrient that one wishes to study – for example eating less than 5 eggs a day – can never be isolated from other behaviours and choices that co-exist in persons who choose to eat less (or more) than 5 eggs a day. Simply put a person eating 6 eggs a day is likely to be unusual in many ways other than just her devotion to eating eggs. And as a result of her egg addiction, what foods does she choose to avoid and how might that choice of avoidance also influence her long-term health? For the evidence clearly establishes that healthy people make a range of healthy choices – they tend to eat the diet that they are told is healthy; they exercise regularly and they avoid smoking and excessive weight gain. How is one ever to know if their health is the result of their exercising and avoidance of weight gain and smoking, rather than their choice to avoid eating a particular nutrient in excess? Indeed it is not impossible that their “healthy” diet might actually be unhealthy, if this harmful effect is obscured by the overriding benefits of exercise, leanness and not smoking. The point is that we cannot continue to justify giving dietary advice based solely on the findings only from longitudinal associational studies that cannot prove causation. Especially when the more vigorously we have championed that advice, the more rapidly has the obesity/T2DM epidemic grown into a global pandemic. Indeed I argue that the very reason we are facing an uncontrollable global diabetes/obesity pandemic at the moment, is because we have promoted dietary guidelines that are based solely on “evidence” from associational studies without acknowledging that RCTs have either not supported those conclusions or might have actively disproved them. The solution in my mind is that we need to give dietary advice to persons with diabetes, T2DM especially, based on our understanding of the underlying patho-physiology of the condition, not on false information provided by associational epidemiological studies that are unable to prove causation. I suggest that we know a number of features of the abnormal biology of T2DM with absolutely certainty. And these are: 1. Persons with T2DM are intolerant of carbohydrate. Thus it makes sense to restrict their dietary carbohydrate intakes as much as possible. 2. Persons with T2DM are intolerant of carbohydrates because they have insulin resistance. Which requires that they continually over-secrete insulin in response to carbohydrate (and to a lesser extent protein ingestion). Thus T2DM is a disease of insulin excess (hyperinsulinaemia). The multitude of complications that develop in this condition, most especially the obstructive arterial disease, are a result of this hyperinsulinaemia (and associated non-alcoholic fatty liver disease – NAFLD). 3. Persons with T2DM treated with insulin have a poorer long-term outcome than those who use little or no insulin. This is because more insulin (either secreted internally from the pancreas or injected) worsens the underlying insulin resistance setting up a vicious cycle: More insulin resistance requires more insulin that in turn produces more insulin resistance, worsening the T2DM. 4. Thus the goal of treatment in T2DM (as in Type I diabetes mellitus (T1DM)) must be to minimize the use of insulin, either secreted internally or injected. Dietary intervention in the form of a very restricted carbohydrate intake with a moderate protein intake and a high intake of healthy fats will minimize insulin secretion and reduce hyperinsulinaemia. This is the type of diet that was used in all children with T1DM before the discovery of insulin in the early 1920s. 5. Of the three dietary macronutrients, only dietary carbohydrates are non-essential. Thus it is established that the minimal daily dietary requirement for carbohydrate is zero grams per day. 6. Even in persons with T2DM eating 25-50g carbohydrate/day, the liver produces an excess of glucose (from protein and fat). As a result blood glucose concentrations are elevated in T2DM – one of the diagnostic hallmark features of the disease. 7. The statement that glucose is the sole fuel for human brain activity is false – the brain has a great capacity to use alternate fuels, both ketones and lactate for its energy needs. The corollary that persons with T2DM must eat carbohydrates to insure adequate brain function is also false. In fact brain glucose uptake is already maximal at a blood glucose concentration of 1.5mmol/L whereas blood glucose concentrations even in T2DM patients eating 25-50g carbohydrate/day is seldom less than 5mmol/L. 8. Both in healthy normals and in persons with T2DM, the single most important determinant of the blood glucose concentration and especially the rise after meals, including the rise in blood insulin concentrations, is the amount of glucose delivered from the gut. Which in turn is a direct function of the amount of carbohydrate that is ingested. 9. Thus it makes absolute sense that the crucial intervention to regulate blood glucose (and insulin) concentrations in persons with T2DM, is to limit the amount of carbohydrate they are advised/allowed to eat. Intermittent fasting is another technique to insure that blood insulin concentrations remain low. 10. My father did not die (nor will I) because his brain was not receiving enough glucose. He died because he developed disseminated obstructive arterial disease. Thus the prevention of the fatal complications in T2DM requires that we understand what causes arterial disease in T2DM. 11. The arterial damage that occurs in T2DM is due to a continual state of hyperinsulinaemia associated with abnormalities in blood glucose and lipid concentrations, the latter caused by NAFLD. The key blood markers of this atherogenic dyslipidaemia are the following:
Thus it seems clear to me what diets we who have T2DM should be following. It surely is not rocket-science! On the basis of this hard scientific evidence, I have made my choice. But I am always open to modification, should new information, based on credible scientific evidence from appropriately robust scientific methods, show there is an even better way. Reference: Freemantle S. Diabetes: A Global Epidemic. Longevity. July 2016, pp 37-48.
Source: http://foodmed.net/2016/07/06/noakes-do-doctors-dietitians-make-diabetes-a-threat-to-life/ 
Eating healthily all the time can be a big challenge. With 57 per cent of women and 67 per cent of men in the UK now overweight, it’s clear that conventional dietary advice isn’t working. Our obesity epidemic is out of control — and although we try our best to ‘eat less and exercise more’, we are only getting sicker and fatter. All that received wisdom has succeeded in doing is to fuel a billion-pound diet industry, while turning us into a nation of sugar-guzzling, disillusioned yo-yo dieters. But pioneering academics and medics in the U.S. and South Africa have compiled a mountain of research to show that the endlessly promoted low-fat, carbohydrate-based diet recommended by dietitians and nutritionists around the world is not only ineffectual, but may in fact be to blame for making us fat and unhealthy. They now believe that, regardless of our weight, we should all be eating MORE fat, not less, and cutting back severely on carbohydrates — particularly sugar. In Saturday’s paper, leading British cardiologist Dr Aseem Malhotra set out the case for a radical change of thinking to embrace a low-carbohydrate diet high in healthy fats as the key to ending our obesity epidemic and slowing the escalation of diabetes and heart disease. All this week, the Daily Mail is serializing a new book by Karen Thomson, the great-granddaughter of pioneering South African heart surgeon Dr Christiaan Barnard. You could lose as much as a stone in a month without cravings or hunger, and set yourself up for a lifetime of healthy eating — without ever having to worry about dieting againKaren, like Dr Malhotra, believes a low-carb, healthy fat diet (LCHF) is the most beneficial way to eat. She is convinced this is the only safe route out of the sugar addiction that hinders so much of our healthy eating resolve — and that it’s the key to losing weight, staying slim and feeling fabulous forever. In today’s paper, we outline the fundamentals and get you started on your weight-loss journey with a five-day meal plan and delicious recipes to entice you into a new LCHF way of life. Over the coming days, we’ll give you tips and tricks to stay at it — and delicious daily recipes so you’ll never feel hungry. You could lose as much as a stone in a month without cravings or hunger, and set yourself up for a lifetime of healthy eating — without ever having to worry about dieting again The Effortless Way To Beat Cravings The new approach is all about re-thinking what you eat and it starts with the simplest of steps: cutting down sugar-rich foods in your diet. Even if we don’t realize it, most of us eat 22 teaspoons of sugar a day — that’s 350 empty calories our bodies don’t need. Remove it and we’d all be on course for effortless slenderness. Simple? Well, not quite. Sugar has a sting in its tail. It is highly addictive. The sugar-rich, carbohydrate-heavy diet on which so many of us have depended for decades plus the proliferation of sugary snacks available and the power of advertising by big food manufacturers have left many of us hooked on sugar and starchy foods. With these so much a part of our lives, quitting completely can seem impossible — but that’s the sugar talking. Over the coming days, we will show you how to do it. Even if carbohydrates have been the staple of your diet since you were a child, and if sweets are your reward, chocolate your treat and puddings your joy, you CAN do this. Diet That Makes You Slim And Healthy The healthiest and easiest way to quit sugar and lose weight is to adopt a diet low in carbohydrates and high in healthy fats. Although this is diametrically opposed to much conventional dietary advice, it is a medically accepted regimen, which is gaining interest and gathering expert backing across the world. It has a massive social media following, with highly respected medics arguing that it is the ONLY healthy way to lose weight and protect against diabetes and heart disease. To take one example, respected American dietary expert Dr Gary Taubes recently argued that tackling obesity isn’t about changing how much you eat, but what you eat. He and many other experts all now believe that LCHF is the answer. THE GOLDEN RULES TO MAKE THE LOW-CARB HEALTHY-FAT DIET SO SIMPLE The Low-Carb Healthy-Fat diet (LCHF) is designed to keep carbohydrate intake low, depending on how active you are and how quickly you want to lose weight. If getting slimmer, rather than general health, is your first concern, use weight loss mode (below) as your model, switching to health mode when your aim has been achieved.
In its modern incarnation, it was designed not as a short-term ‘miracle weight loss’ program, but as a long-term healthy way to eat. Yet the bonus people have found is that they can lose up to a stone in a month, without counting calories and without feeling hungry. This is because our bodies process the foods we eat in different ways. With a typical carbohydrate-based diet, carbs are converted into blood sugar, which your body burns for energy. Any excess sugar is converted to fat (under instruction from the hormone insulin) and stored away. But if you restrict carbohydrates to 30-50g a day or less, your body can no longer get the energy it needs from sugars, so it has to bring in other mechanisms and fuels. This is where fat comes in. You can get all the energy you need from fat stored around your body and from the fat in your food — there is very little physiological need for carbohydrates, and no place for sugar at all. It's a good idea to practice portion control for proteins and fats, and lower your intake of ‘dense’ or starchy vegetables. The key to harnessing LCHF for weight loss is keeping your total carbohydrates below 30-50g a day. This liberates the body from the tyranny of sugar addiction and helps you lose excess weight naturally. But cutting right down on carbohydrates isn’t easy, unless you stock up on healthy fats to silence cravings and keep you feeling full. If you’re active — that is, you exercise regularly or your job keeps you on your feet — or you’re happy about your weight, you should be able to tick along on a higher carbohydrate intake — up to 80 g a day — and still reap the banting benefits. But the plan only works if your carbohydrates come not from pasta, rice, bread and doughnuts, but from whole foods such as vegetables, pulses and fruits, which are packed with nutrients and which your body metabolizes slowly. The good news is, you won’t need to count calories. The new balance of nutrients and healthy fats in your diet should mean you’re not plagued by cravings. But if you’re a sugar addict, your body could be well-practiced at overriding natural satiety (fullness) signals. If you suspect you might have addiction issues, you will need to re-teach yourself to listen and monitor matters until your dietary intake is back under your body’s natural control. To succeed, you need to reappraise old ideas about nutrition. Fabulous Fats To adapt to having no sugar and far fewer carbs in your life, you have to put something back — and this is likely to mean eating more healthy fats than you were used to. It might seem counter-intuitive if you want to lose weight but fats slow digestion, keeping you feeling full. They are your secret weapon against sugar cravings. And plenty of respected studies now show that most fats — even saturated fats — are very, very good for your health. This dietary change is what many people find hardest to get their heads around — but don’t go crazy and ignore the portion size suggestions above. If you graze on nuts or tuck into tubs of yoghurt all day, you will consume too many calories for the diet’s weight-loss effects to work. Yet if you follow the advice on these pages, you can start slimming — and feeling fabulous — in no time. If you have diabetes or high blood pressure or are on any form of medication, check with your GP before making any dietary changes. There’s lots of research to show an LCHF diet brings blood pressure down if it’s high and can help to normalize blood sugar levels if you have diabetes (type 1 or 2). So keep a close eye on your blood pressure and blood sugar levels and be prepared to adjust your medication accordingly. Don’t do this without consulting your GP. Read more: http://www.dailymail.co.uk/femail/food/article-3672595/Cut-carbs-quit-sugar-feel-fabulous-s-food-revolution-ll-make-slimmer-happier-s-blissfully- Is there enough scientific evidence supporting the 2015 Dietary Guidelines for Americans? Not according to this article:
ResearchGate: Problems with the 2015 Dietary Guidelines for Americans For example there’s no sound evidence for allowing about half of all grains to be refined (!) or for the truly old and moldy recommendation to eat low-fat dairy and to avoid natural saturated fats. There’s even is a great risk that these guidelines lead to higher risk of diseases such as cardiovascular disease, cancer, obesity, diabetes etc. This means that you’re likely better off going against the recommendations by consuming natural foods such as meat, fish, eggs, natural fats and vegetables, rather than foods low in saturated fats and sodium, but full of grains and industrial oils. Source: http://www.dietdoctor.com/problems-american-dietary-guidelines When Wendy Pogozelski began studying the primary literature in the field of nutrition, she was shocked to find enormous differences between the nutrition advice she’d found in the mainstream vs. the research and clinical results she was reading about. She connected with other researchers, doctors, biochemists and professors who had similar concerns and has become part of an international effort to help students, consumers and patients understand the science behind nutrition. Dr. Wendy Pogozelski received her B.S. in Chemistry from Chatham University and her PhD from The John Hopkins University. She was an Office of Naval Research post-doctoral fellow at the Naval Research Lab in Washington, D.C. In 1996, she came to Geneseo where she now holds the rank of Distinguished Teaching Professor and serves as Chair of the Chemistry Department. In her laboratory work, Dr. Pogozelski and her students investigate the effects of radiation on mitochondria. Since developing an interest in the biochemistry of nutrition, Dr. Pogozelski has been working with an international group of scientists and clinicians who are trying to bridge the gulf between scientific research and nutrition education. Think about this, what kind of pressure are we exerting on our health each and every day? What is the effect of the food choices we make... or don’t make? Nick Murphy, owner of Mission Fitness, is a Certified Personal Trainer and Life Coach. He has 20+ years of experience in his field and is equipped to train clients across the fitness spectrum from the world-class athlete to the morbidly obese, and everyone in between. His passion is to teach people about health, fitness, diet and exercise, and to empower clients to take control of their lives.  I recently wrote a couple of posts explaining that over the years, I’ve revised my explanation of “the alternative hypothesis” from this: More Carbohydrates => Higher Insulin => Fat Storage to this: Damaging Diet => Hormonal Disruption => Fat Storage It’s not the biologically beneficial rise in insulin after a meal that makes people obese, I said in those posts. It’s chronically high insulin (along with other hormonal disruptions) resulting from a bad diet. In comments, a few of you suggested I read Dr. Jason Fung’s book The Obesity Code because it expresses similar ideas. Good suggestion. It’s an enlightening and very readable book – meaning it passes my “Aunt Martha” test. Your Aunt Martha could read this book without giving up because she doesn’t want to keep a medical dictionary on her desk. As I expected, insulin is still front and center in Fung’s explanation of why we get fat. In fact, the book’s cover includes the subhead Why your body’s own insulin is the key to controlling your weight. After citing plenty of research to effectively dismiss the “it’s all about consuming too many calories” explanation of obesity in the early chapters, Fung begins chapter seven like this: I can make you fat. Actually I can make anyone fat. How? By prescribing insulin. It won’t matter that you have willpower, or that you exercise. It won’t matter what you choose to eat. It’s simply a matter of enough insulin and enough time. Wait … hasn’t Dr. Fung read on the internet that we mustn’t blame insulin because it’s actually a wunnerful, wunnerful appetite suppressant? Well, perhaps he has … but if so, I’m sure he laughed. He has years of clinical experience with the stuff, as he explains in the book’s introduction: I’ve often watched patients start insulin treatment for their diabetes, knowing that most will gain weight. “Doctor,” they say, “you’ve always told me to lose weight. But the insulin you gave me makes me gain so much weight. How is this helpful?” … Like many doctors, I believed that weight gain was caloric imbalance – eating too much and moving too little. But if that were so, why did the medication I prescribed – insulin – cause such relentless weight gain? Fung answers his own question in chapter seven: Everything about human metabolism, including the body set weight, is hormonally regulated. A critical physiological variable such as body fatness is not left up the vagaries of daily caloric intake and exercise. Instead, hormones precisely and tightly regulate body fat. We don’t consciously control our body weight any more than we control our heart rates, our basal metabolic rates, our body temperatures or our breathing. But it isn’t just about insulin. Fung includes chapters on cortisol (which triggers weight gain partly by raising insulin) and other hormones, such as leptin, that are involved in weight regulation. And insulin isn’t just about how many grams of carbohydrate we consume. As Fung writes in chapter nine: The carbohydrate-insulin hypothesis, the idea that carbohydrates cause weight gain because of insulin secretion, was not exactly wrong. Carbohydrate-rich foods certainly do increase insulin levels to a greater extent than the other macronutrients. High insulin certainly does lead to obesity. However, the hypothesis stands incomplete. There are many problems, with the paradox of the Asian rice eater being the most obvious. … Indeed, many primitive societies that ate mostly carbohydrates have low obesity rates. In 1989, Dr. Staffan Lindeberg studied the residents of Kitava, one of the Trobriand Isands in Papua New Guinea’s archipelago – one of the last places on Earth where people ate a largely traditional diet. Starchy vegetables, including yam, sweet potato, taro and cassava, made up the basis of their diet. It isn’t foods that raise insulin that make us fat, Fung explains in the following chapters. It’s foods that lead to insulin resistance. Once we become insulin resistant, the entire hormonal system goes out of whack. Fung spends the next few chapters describing the foods that likely make us insulin resistant (sugar being a primary culprit) and how insulin resistance makes us fat. Insulin resistance is largely about what we eat. But rolling back the effects – and perhaps preventing insulin resistance in the first place – is also about when we eat. That was the most useful message in the book for me, since I’ve already read rather a lot about the effects of foods. As Fung explains, insulin is supposed to rise after meals. But then it’s supposed to drop and stay low for several hours. Back when few Americans were overweight, that’s what happened — because we ate three meals per day, period. Now we add constant snacking into the mix. When I was shooting interviews for Fat Head, Dr. Eric Oliver, author of Fat Politics, said that while people like Morgan Spurlock want to blame obesity on restaurants for serving larger meals, the real problem seems to be how often we eat between meals. Fung explains why that’s such a problem: The balance between the fed state (insulin dominant) and the fasted state (insulin deficient) has been completely destroyed. We are now spending most of our time in the fed state. … We are taught to eat the moment we roll out of bed. We are taught to eat throughout the day and again just before we sleep. We spend up to 18 hours in the insulin-dominant state, with only six hours insulin-deficient. A lousy diet, of course, makes snacking irresistible. Refined carbs jack up your blood sugar, and your body responds by flooding your bloodstream with enough insulin to give you low blood sugar. If you work in an office, I’m sure you’ve seen exactly what Fung is describing. I see people eat their white-bread sandwiches at noon, and by 3:30 they’re back in the cafeteria, trying to decide if they should raise blood sugar with a candy bar, a bag of chips, or some microwaved popcorn. Fung describes this as the vicious cycle that leads to insulin resistance. When insulin is too high, too often, cells down-regulate their insulin receptors. Then the body cranks out more insulin to try to lower high blood sugar. Then we get fatter. And hungrier. And snack more often. Part of the cure is real food, and Fung devotes a good chunk of the book to the topic. But another part of the cure is to dial back insulin resistance through intermittent fasting. As you know, I’m a fan of the Wisdom of Crowds. Fung reminds the reader that in nearly all ancient cultures, periodic fasting was considered a boon to good health. It was part of their wisdom. In the final chapter, Fung lays out the why and the how of intermittent fasting. Here’s part of the why: To break the insulin-resistance cycle, we must have recurrent periods of very low insulin levels. But how can we induce our body into a temporary state of very low insulin levels? We know that eating the proper foods prevents high levels, but it won’t do much to lower them. Some foods are better than others; nonetheless, all foods increase insulin production. If all foods raise insulin, then the only way for us to lower it is to completely abstain from food. The answer we are looking for is, in a word, fasting. In the rest of chapter, Fung describes the hormonal effects of fasting and dispels the many myths about going without food … such as “it will depress your metabolism.” Interestingly, the research he cites here and in other chapters shows that while living on a low-calorie, low-fat diet will indeed slow down your metabolism, periodic fasting doesn’t. Apparently we’re built for it. Given that paleo man’s hunts weren’t already successful, that makes sense. Jimmy Moore and Dr. Fung are co-authoring a book titled Fasting Clarity that’s scheduled to be published later this year. I’m looking forward to reading the expanded version of this topic. Source: http://www.fathead-movie.com/index.php/2016/06/27/review-the-obesity-code/ There may be a valid rationale to use potassium citrate as a supplement for those who are interested in improving beta cell function (i.e. diabetes) and insulin sensitivity.
Although the sample size is small, the research method for “Effects of potassium citrate or potassium chloride in patients with combined glucose intolerance: A placebo-controlled pilot study”, seems to hold its own. Conen K. et al., conducted this double-blind, placebo-controlled study with 7 males and 4 females ages 47-63 years old who were glucose intolerant (an umbrella term for metabolic conditions which result in higher than normal blood glucose. Pre-diabetes, type 2 diabetes, impaired fasting glucose and impaired glucose tolerance is defined by the World Health Organization as a fasting blood sugar level of 6.0 mmol/l) and found that both systolic and diastolic blood pressure, beta cell function and insulin sensitivity were significantly and positively affected when given 90 meqs of potassium citrate when compared with potassium chloride. They concluded that the citrate anion (The first intermediate of the citric acid or Krebs cycle, it plays an important role for fatty acids and it acts as a carrier for acetyl-CoA, and then synthesis for fatty acids.) is responsible for the insulin-sensitizing and blood pressure lowering results. Yet potassium itself may be more than a viable piece of the diabetes/insulin resistance treatment puzzle. One’s own genetic mutations (KCNJ11 gene and KCNQ1 (specific to the Asian population) affect potassium channels that influence insulin secretion, http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3197792/. Potassium:
Potassium researchers recommend a diet that maintains an optimal sodium-to-potassium ratio of 1:5 or less, http://www.anaturalhealingcenter.com/documents/Thorne/monos/Potassium%20mono.pdf. Potassium recommendations for adolescents and adults is 4,700 mg/day, for children: 1 to 3 years of age is 3,000 mg/day, 4 to 8 years of age is 3,800 mg/day and 9 to 13 years of age is 4,500 mg/day. Foods that are good sources of potassium include: salmon, tuna, turkey, clams, avocado, white mushrooms, spinach, kale Swiss chard, collards, broccoli, blackberries, cantaloupe, grapefruit, artichokes and tomato. If you are not able to meet potassium recommendations, using a supplement seems prudent. There are certain population groups like the elderly, pregnant women or children, those with kidney issues, ulcers or anyone prone to metabolic alkalosis that should not use potassium supplements. Any nutrient supplementation should be supervised by a doctor. If potassium citrate can work as an insulin sensitizer while preserving beta cell function, it, along with other natural supplements like magnesium and chromium should be considered a first line option in diabetes treatment before using pharmaceutical drugs that have long lasting and more severe consequences. Source: https://valerieberkowitz.wordpress.com/2016/06/27/the-potassium-tie-in-to-insulin-sensitivity/ Introduction Ketosis is an often misunderstood subject. Its presence is thought to be equal to starvation or a warning sign of something going wrong in your metabolism. But nothing could be farther from the truth, except if you are an ill-treated type 1 diabetic person.[1] Ketones – contrary to popular belief and myth – are a much needed and essential healing energy source in our cells that come from the normal metabolism of fat. The entire body uses ketones in a more safe and effective way than the energy source coming from carbohydrates – sugar AKA glucose. Our bodies will produce ketones if we eat a diet devoid of carbs or a low carb diet (less than 60 grams of carbs per day).[2] By eating a very low carb diet or no carbs at all (like a caveman) we become keto-adapted. In fact, what is known today as the ketogenic diet was the number one treatment for epilepsy until Big Pharma arrived with its dangerous cocktails of anti-epileptic drugs. It took several decades before we heard again about this diet, thanks in part to a parent who demanded it for his 20-month-old boy with severe seizures. The boy’s father had to find out about the ketogenic diet in a library as it was never mentioned as an option by his neurologist. After only 4 days on the diet, his seizures stopped and never returned.[3] The Charlie Foundation was born after the kid’s name and his successful recovery, but nowadays the ketogenic diet is available to the entire world and it’s spreading by word of mouth thanks to its healing effects. It is not only used as a healthy lifestyle, it is also used for conditions such as infantile spasms, epilepsy, autism, brain tumors, Alzheimer’s disease, Lou Gehrig’s disease, depression, stroke, head trauma, Parkinson’s disease, migraine, sleep disorders, schizophrenia, anxiety, ADHD, irritability, polycystic ovarian disease, irritable bowel syndrome, gastroesophageal reflux, obesity, cardiovascular disease, acne, type 2 diabetes, tremors, respiratory failure and virtually every neurological problem but also cancer, and conditions where tissues need to recover after a loss of oxygen.[4] Our body organs and tissues work much better when they use ketones as a source of fuel, including the brain, heart and the core of our kidneys. If you ever had a chance to see a heart working in real time, you might have noticed the thick fatty tissue that surrounds it. In fact, heart surgeons get to see this every day. A happy beating heart is one that is surrounded by layers of healthy fat. Both the heart and the brain run at least 25% more efficiently on ketones than on blood sugar. Ketones are the ideal fuel for our bodies unlike glucose – which is damaging, less stable, more excitatory and in fact shortens your life span. Ketones are non-glycating, which is to say, they don’t have a caramelizing ageing effect on your body. A healthy ketosis also helps starve cancer cells as they are unable to use ketones for fuel, relying on glucose alone for their growth. [5]The energy producing factories of our cells – the mitochondria – work much better on a ketogenic diet as they are able to increase energy levels in a stable, long-burning, efficient, and steady way. Not only that, a ketogenic diet induces epigenetic changes[6] which increases the energetic output of our mitochondria, reduces the production of damaging free radicals, and favours the production of GABA – a major inhibitory brain chemical. GABA has an essential relaxing influence and its favored production by ketosis also reduces the toxic effects of excitatory pathways in our brains. Furthermore, recent data suggests that ketosis alleviates pain in addition to having an overall anti-inflammatory effect. [7] The ketogenic diet acts on multiple levels at once, something that no drug has been able to mimic. This is because mitochondria are specifically designed to use fat for energy. When our mitochondria use fat as an energetic source, its toxic load is decreased, the expression of energy producing genes are increased, its energetic output is increased, and the load of inflammatory energetic-end-products is decreased. The key of these miraculous healing effects relies on the fact that fat metabolism and its generation of ketone bodies (beta-hydroxybutyrate and acetoacetate) by the liver can only occur within the mitochondrion, leaving chemicals within the cell but outside the mitochondria readily available to stimulate powerful anti-inflammatory antioxidants. The status of our mitochondria is the ultimate key for optimal health and while it is true that some of us might need extra support in the form of nutritional supplementation to heal these much needed energy factories, the diet still remains the ultimate key for a proper balance. Our modern world’s staple energetic source is sugar which needs to be processed first in the cell soup before it can be passed into the energy factory of the cell- the mitochondrion. Energy sources from fat don’t require this processing; it goes directly into the mitochondria for energetic uses. That is, it is more complicated to create energy out of sugar than out of fat. As Christian B. Allan, PhD and Wolfgang Lutz, MD said in their book Life Without Bread: Carbohydrates are not required to obtain energy. Fat supplies more energy than a comparable amount of carbohydrate, and low-carbohydrate diets tend to make your system of producing energy more efficient. Furthermore, many organs prefer fat for energy.The fact is you get MORE energy per molecule of fat than sugar. How many chronic and autoimmune diseases have an energy deficit component? How about chronic fatigue? Fibromyalgia? Rheumatoid Arthritis? Multiple Sclerosis? Cancer? Back to Allan and Lutz: Mitochondria are the power plants of the cell. Because they produce most of the energy in the body, the amount of energy available is based on how well the mitochondria are working. Whenever you think of energy, think of all those mitochondria churning out ATP to make the entire body function correctly. The amount of mitochondria in each cell varies, but up to 50 percent of the total cell volume can be mitochondria. When you get tired, don’t just assume you need more carbohydrates; instead, think in terms of how you can maximize your mitochondrial energy production…If you could shrink to a small enough size to get inside the mitochondria, what would you discover? The first thing you’d learn is that the mitochondria are primarily designed to use fat for energy! In short, let fat be thy medicine and medicine be thy fat! You will think that with all of this information we would see ketogenic diets recommended right and left by our health care providers, but alas, that is not the case. Mainstream nutritionists recommend carbohydrates AKA sugar as the main staple of our diets. The problem with this (and there are several of them) is that in the presence of a high carb diet we are unable to produce ketones from the metabolism of fats, thus, depriving our bodies from much healing ketone production. The fact that we live in a world which uses glucose as a primary fuel means that we eat a very non healing food in more ways than one. I have been doing the low carb diet for about a week and a half now and I must say, I am really starting to feel amazing!!! The first few days my head hurt, I felt lethargic, and my legs felt so heavy. But after I got past that, I have so much energy. I don’t get tired anymore around 3pm. The best part is, I am not constantly thinking and obsessing about food. I feel a real sense of inner calm. My skin looks better, my hair looks better too. I have been having bacon and eggs for breakfast, a pork chop or other piece of meat for lunch, and usually some pork and sometimes some green beans for dinner. I have also lost some weight! Woo hoo!!! -Angela, United States. Sott.net forum. We have been on a ketogenic diet for nearly three million years and it has made us human. It was the lifestyle in which our brains got nurtured and evolved. But not anymore, unless we all make an effort to reclaim this lost wisdom. Nowadays the human brain is not only shrinking, but brain atrophy is the norm as we age and get plagued with diseases such as Alzheimer’s disease, Parkinson’s disease, senile dementia and so forth. In the mean time new research is starting to elucidate the key role of our mitochondria in the regulation of the cell cycle – the vital process by which a single celled fertilized egg develops into a mature organism, as well as the process by which hair, skin, blood cells, and some internal organs are renewed. In the complicated and highly choreographed events surrounding cell-cycle progression, mitochondria are not simple bystanders merely producing energy but instead are full-fledged participants.[8] Given the significant amount of energy needed to make all the nutrients required for cell division, it makes sense that some coordination existed. This long ignored and overlooked connection between the mitochondria and the cell cycle is something that is worthy of considerably more attention as we understand the role of diet in our bodies. We’ll have to take a closer look at this subject of ketosis, as it really holds the key to unlock our transformational pathways that will lead us to an outstanding healthy living. Mitochondrial Dysfunction Mitochondria are best known as the powerhouses of our cells since they produce the cell’s energy. But they also lead the genetic orchestra which regulates how every cell ages, divides, and dies. They help dictate which genes are switched on or off in every single cell of our organism. They also provide the fuel needed to make new brain connections, repair and regenerate our bodies. Whether we are housewives, sportsmen or labourers, energy is a topic that concerns us all, every day and in every way. Our well being, behaviour and ability to perform the tasks put in front of us is all to do with our individual levels of energy. But how do we derive energy from the foods that we eat? There are many man-made myths surrounding energy production in the body and which foods supply energy. Mainstream science says that carbohydrates are what mitochondria use as fuel for energy production. This process is called oxidative metabolism because oxygen is consumed in the process. The energy produced by mitochondria is stored in a chemical “battery”, a unique molecule called adenosine triphosphate (ATP). Energy-packed ATP can then be transported throughout the cell, releasing energy on demand of specific enzymes. In addition to the fuel they produce, mitochondria also create a by-product related to oxygen called reactive oxygen species (ROS), commonly known as free radicals. But what we are not told is that mitochondria were specifically designed to use fat for energy, not carbohydrate. Source: Christian B. Allan, PhD and Wolfgang Lutz, MD, Life Without Bread. There are several very complicated steps in making ATP within mitochondria, but a look at 5 major parts of ATP production will be all that you need to know in order to understand how energy is created within our mitochondria and why fats are the key to optimize their function. Don’t get focused on specific names, just try to see the whole picture. Step 1 – Transportation of Food-Based Fuel Source into the Mitochondria Fuel must first get into the mitochondria where all the action happens. Fuel can come from carbs or it can come from fats. Fatty acids are the chemical name for fat, and medium and large sized fatty acids get into the mitochondria completely intact with the help of L-carnitine. Think of L-carnitine as a subway train that transports fatty acids into the mitochondria. L-carnitine (from the Greek word carnis means meat or flesh) is chiefly found in animal products. Fuel coming from carbs needs to get broken down first outside the mitochondria and the product of this breakdown (pyruvate) is the part that gets transported inside the mitochondria, or it can be used to produce energy in a very inefficient way outside the mitochondria through anaerobic metabolism which produces ATP when oxygen is not present. Step 2 – Fuel is Converted into Acetyl-CoA When pyruvate – the product of breaking down carbs – enters the mitochondria, it first must be converted into acetyl-CoA by an enzymatic reaction. Fatty acids that are already inside the mitochondria are broken down directly into acetyl-CoA in what is called beta-oxidation. Acetyl-CoA is the starting point of the next step in the production of ATP inside the mitochondria. Step 3 – Oxidation of Acetyl-CoA and the Krebs Cycle The Krebs cycle (AKA tricarboxylic acid cycle or citric acid cycle) is the one that oxidizes the acetyl-CoA, removing thus electrons from acetyl-CoA and producing carbon dioxide as a by-product in the presence of oxygen inside the mitochondria. Step 4 – Electrons Are Transported Through the Respiratory Chain The electrons obtained from acetyl-CoA – which ultimately came from carbs or fats – are shuttled through many molecules as part of the electron transport chain inside the mitochondria. Some molecules are proteins, others are cofactors molecules. One of these cofactors is an important substance found mainly in animal foods and it is called coenzyme Q-10. Without it, mitochondrial energy production would be minimal. This is the same coenzyme Q10 that statins drug block producing crippling effects on people’s health. Step 4 is also where water is produced when oxygen accepts the electrons. Step 5 – Oxidative phosphorylation As electrons travel down the electron transport chain, they cause electrical fluctuations (or chemical gradients) between the inner and outer membrane in the mitochondria. These chemical gradients are the driving forces that produce ATP in what is called oxidative phosphorylation. Then the ATP is transported outside the mitochondria for the cell to use as energy for any of its thousands of biochemical reactions. But why is fat better than carbs? If there were no mitochondria, then fat metabolism for energy would be limited and not very efficient. But nature provided us during our evolution with mitochondria that specifically uses fat for energy. Fat is the fuel that animals use to travel great distances, hunt, work, and play since fat gives more energy-packed ATPs than carbs. Biochemically, it makes sense that if we are higher mammals who have mitochondria, then we need to eat fat. Whereas carb metabolism yields 36 ATP molecules from a glucose molecule, a fat metabolism yields 48 ATP molecules from a fatty acid molecule inside the mitochondria. Fat supplies more energy for the same amount of food compared to carbs. But not only that, the burning of fat by the mitochondria – beta oxidation – produces ketone bodies that stabilizes overexcitation and oxidative stress in the brain related to all its diseases, it also causes epigenetic changes that produce healthy and energetic mitochondria and decreasing the overproduction of damaging and inflammatory free radicals among many other things! Mitochondria regulate cellular suicide, AKA apoptosis, so that old and dysfunctional cells which need to die will do so, leaving space for new ones to come into the scene. But when mitochondria function becomes impaired and sends signals that tell normal cells to die, things go wrong. For instance, the destruction of brain cells leads to every single neurodegenerative condition known including Alzheimer’s disease, Parkinson’s disease and so forth. Mitochondrial dysfunction has wide-ranging implications, as the health of the mitochondria intimately affects every single cell, tissue and organ within your body. The catalysts for this destruction is usually uncontrolled free radical production which causes oxidative damage to tissues, fat, proteins, DNA; causing them to rust. This damage, called oxidative stress, is at the basis of oxidized cholesterol, stiff arteries (rusty pipes) and brain damage. Oxidative stress is a key player in dementia as well as autism. We produce our own anti-oxidants to keep a check on free radical production, but these systems are easily overwhelmed by a toxic environment and a high carb diet, in other words, by today’s lifestyle and diet. Mitochondria also have interesting characteristics which differentiate them from all other structural parts of our cells. For instance, they have their own DNA (referred as mtDNA) which is separate from the widely known DNA in the nucleus (referred as n-DNA). Mitochondrial DNA comes for the most part from the mother line, which is why mitochondria is also considered as your feminine life force. This mtDNA is arranged in a ring configuration and it lacks a protective protein surrounding, leaving its genetic code vulnerable to free radical damage. If you don’t eat enough animal fats, you can’t build a functional mitochondrial membrane which will keep it healthy and prevent them from dying. If you have any kind of inflammation from anywhere in your body, you damage your mitochondria. The loss of function or death of mitochondria is present in pretty much every disease. Dietary and environmental factors lead to oxidative stress and thus to mitochondrial injury as the final common pathway of diseases or illnesses. Autism, ADHD, Parkinson’s, depression, anxiety, bipolar disease, brain ageing are all linked with mitochondrial dysfunction from oxidative stress. Mitochondrial dysfunction contributes to congestive heart failure, type 2 diabetes, autoimmune disorders, ageing, cancer, and other diseases. Whereas the nDNA provides the information your cells need to code for proteins that control metabolism, repair, and structural integrity of your body, it is the mtDNA which directs the production and utilization of your life energy. A cell can still commit suicide (apoptosis) even when it has no nucleus nor nDNA. Because of their energetic role, the cells of tissues and organs which require more energy to function are richer in mitochondrial numbers. Cells in our brains, muscles, heart, kidney and liver contain thousands of mitochondria, comprising up to 40% of the cell’s mass. According to Prof. Enzo Nisoli, a human adult possesses more than ten million billion mitochondria, making up a full 10% of the total body weight.[9] Each cell contains hundreds of mitochondria and thousands of mtDNA. Since mtDNA is less protected than nDNA because it has no “protein” coating (histones), it is exquisitely vulnerable to injury by destabilizing molecules such as neurotoxic pesticides, herbicides, excitotoxins, heavy metals and volatile chemicals among others. This increasees free radical production to the extreme which then leads to oxidative stress damaging our mitochondria and its DNA. As a result we get overexcitation of cells and inflammation which is at the root of Parkinson’s disease and other diseases, but also mood problems and behaviour problems. Enough energy means a happy and healthy life. It also reflects in our brains with focused and sharp thinking. Lack of energy means mood problems, dementia, and slowed mental function among others. Mitochondria are intricately linked to the ability of the prefrontal cortex –our brain’s captain- to come fully online. Brain cells are loaded in mitochondria that produce the necessary energy to learn and memorize, and fire neurons harmoniously. The sirtuin family of genes works by protecting and improving the health and function of your mitochondria.[10] They are positively influenced by a diet that is non-glycating, i.e. a low carb diet as opposed to a high carb diet which induces mitochondrial dysfunction and formation of reactive oxygen species. Another thing that contributes to mitochondrial dysfunction is latent viral infection such as the ones of the herpes family. As I mentioned in On Viral “Junk” DNA, a DNA Enhancing Ketogenic Diet, and Cometary Kicks, most, if not all of your “junk” DNA has viral-like properties. If a pathogenic virus takes hold of our DNA or RNA, it could lead to disease or cancer. Herpes simplex virus is a widespread human pathogen and it goes right after our mitochondrial DNA. Herpes simplex virus establishes its latency in sensory neurons, a type of cell that is highly sensitive to the pathological effects of mt DNA damage.[11] A latent viral infection might be driving the brain cell loss in neurodegenerative diseases such as Alzheimer’s disease.[12]As I speculated in Heart attacks, CFS, herpes virus infection and the vagus nerve , a latent herpes virus infection might drive more diseases than we would like to admit. Members of the herpes virus family (i.e. cytomegalovirus and Epstein-Barr virus which most people have as latent infections!), can go after our mitochondrial DNA, causing neurodegenerative diseases by mitochondrial dysfunction. But a ketogenic diet is the one thing that would help stabilize mtDNA since mitochondria runs the best on fat fuel. As it happens, Alzheimer’s disease is the one condition where a ketogenic diet has its most potential healing effect.[4] The role of mitochondrial dysfunction in our “modern” age maladies is a staggering one. Optimal energetic sources are essential if we are to heal from chronic ailments. It is our mitochondria which lies at the interface between the fuel from foods that come from our environment and our bodies’ energy demands. And it is a metabolism based on fat fuel, a ketone metabolism, the one which signals epigenetic changes that maximizes energetic output within our mitochondria and help us heal. I am incredulous at how my body is responding. I think I am totally carb intolerant. I’ve struggled with extreme fatigue/exhaustion for so many years, even with improved sleep in a dark room that I can’t tell you how wonderful it is to wake up in the morning, get out of bed and not long to crawl back in, going through the day by will mostly. Also chronic long-standing intestinal issues are finally resolving. A couple of people at work have made comments to the effect that I’m a “different woman”, calmer, no more 'hyperness' under pressure, stress seems to roll off of my back as well. I’ve lost a little weight and although I don’t weigh myself, my clothes are definitely looser. I’ve had the round middle for so many years I was resigned to struggling to bend over to pull my shoes on! -Bluefyre, 56 years old, United States. Sott.net forum Ketosis – Closer Look The presence of ketones in the blood and urine, a condition known as ketosis, has always been regarded as a negative situation, related to starvation. While it is true that ketones are produced during fasting, ketones are also produced in times of plenty, but not plenty of carbohydrates since a carb metabolism suppresses ketosis. In the absence of most carbs in the diet, ketones will form from fat to supply energy. This is true even if lots of fats and enough protein are eaten, something that is hardly a starvation condition. As we already saw, a ketogenic diet has been proved useful in a number of diseases, especially neurological ones. Strictly speaking, a ketogenic diet is a high fat diet in which carbohydrates are either completely eliminated or nearly eliminated so that the body has the very bare minimum sources of glucose. That makes fats (fatty acids) a mandatory energetic fuel source for both the brain and other organs and tissues. If your carb intake is high, you’ll end up storing both the fat and the carbs in your fat tissue thanks to the hormone insulin. A ketogenic diet is not a high protein diet, which as it happens, can also stimulate insulin. It is basically a diet where you rely primarily on animal foods and especially their fats. I recently had my annual blood work done (cholesterol, etc.) During the review, my doctor said that everything looked great! He then encouraged me to continue on my great ‘low fat, high fruit and veggie diet’ that I must be following! I just smiled. Next visit I’m going to tell him about my real ‘diet’. Lol -1984, United States. Sott.net forum. Among the by-products of fat burning metabolism are the so called ketone bodies – acetoacetate, β-hydroxybutyrate and acetone – which are produced for the most part by the liver. When our bodies are running primarily on fats, large amounts of acetyl-CoA are produced which exceed the capacity of the Krebs cycle, leading to the making of these three ketone bodies within liver mitochondria. Our levels of ketone bodies in our blood go up and the brain readily uses them for energetic purposes. Ketone bodies cross the blood brain barrier very readily. Their solubility also makes them easily transportable by the blood to other organs and tissues. When ketone bodies are used as energy, they release acetyl-CoA which then goes to the Krebs cycle again to produce energy. In children who were treated with the ketogenic diet to treat their epilepsy, it was seen that they become seizure-free even long after the diet ended, meaning that not only did the diet proved to be protective, but also it modified the activity of the disease , something that no drug has been able to do.[13] In Alzheimer’s disease, as levels of ketone bodies rise, memory improves. People’s starved brains finally receive the much needed fats they need! In fact, every single neurological disease is improved on the ketogenic diet. The benefits of a ketogenic diet can be seen as quickly as one week, developing gradually over a period of 3 weeks. There are several changes in gene expression involving metabolism, growth, development, and homeostasis among others. The hippocampus is a region in your brain that is very vulnerable to stress which makes it lose its brain cells. The hippocampus has to do with memory, learning, and emotion. As it happens, a ketogenic diet promotes the codification of genes which creates mitochondria in the hippocampus, making more energy available. A larger mitochondrial load and more energy means more reserve to withstand much more stress.[14] In some animal models, following a ketogenic diet, there is a 50% increase in the total number of mitochondria in the hippocampus, resulting in more brain ATP.[15] Other animal studies show how communication between brain cells in the hippocampus would remain smooth for 60% longer when exposed to a stressful stimulus compared to their counterparts who didn’t had a ketogenic diet.[16] This is very important since too much stress can damage the hippocampus and its capacity to retrieve information, making you “absent-minded” or “brain-scattered”, as well as affecting the ability of your prefrontal cortex to think and manage behavior. A ketogenic diet also increases levels of the calming neurotransmitter – GABA - which then serves to calm down the overexcitation which is at the base of major neuro-degenerative diseases, but also anxiety and other mood problems. A ketogenic diet also increases antioxidant pathways that level the excess production of free radicals from a toxic environment. It also enhances anti-inflammatory pathways. Ketosis also cleans our cells from proteins that act like “debris” and which contribute to ageing by disrupting a proper functioning of the cell.[17] It basically does this by what is known as autophagy which preserves the health of cells and tissues by replacing outdated and damaged cellular components with fresh ones. This prevents degenerative diseases, ageing, cancer, and protects you against microbial infections. A ketogenic diet not only rejuvenates you, it also makes a person much less susceptible to viruses and bacterial infections.[18] This is very relevant due to the increasing number of weird viral and bacterial infections that seem to be incoming from our upper atmosphere[19] (for more information see New Light on the Black Death: The Viral and Cosmic Connection), or due to high levels of radiation that creates more pathogenic strains (see Detoxify or Die: Natural Radiation Protection Therapies for Coping With the Fallout of the Fukushima Nuclear Meltdown). Either way, we are more vulnerable than ever due to the state of our mitochondria. But we can prepare for the worst with ketosis. Ketone-enhanced autophagy is very important because autophagy can target viruses and bacteria that grow inside cells which are very problematical.[20] Intracellular viruses and bacteria can lead to severe mitochondrial dysfunction and ketosis remains by far our best chance against them. A Paoli, A Rubini, J S Volek and K A Grimaldi. Beyond weight loss: a review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets. European Journal of Clinical Nutrition (2013) 67, 789–796 Ketone bodies production through intermittent fasting and the ketogenic diet is the most promising treatment for mitochondrial dysfunction.[21]The longevity benefits seen by caloric restriction research is due to the fact that our bodies shift to a fat burning metabolism within our mitochondria. With a ketogenic diet, we go into a fat burning metabolism without restricting our caloric intake.
Ketosis deals effectively with all the problems of a diet rich in carbs – the one recommended by mainstream science. Namely a ketogenic diet deals with anxiety, food cravings, irritability, tremors, and mood problems among others. It is a crime to discourage the consumption of a high fat diet considering that a ketogenic diet shrinks tumours in human and animal models, and enhances our brain’s resilience against stress and toxicity. In addition to increasing the production of our body’s natural valium – GABA – the increased production of acetyl-CoA generated from the ketone bodies also drives the Krebs cycle to increase mitochondrial NADH (reduced nicotinamide adenine nucleotide) which our body uses in over 450 vital biochemical reactions – including the cell signalling and assisting of the ongoing DNA repair. Because the ketone body beta-hydroxybutyrate is more energy rich than pyruvate, it produces more ATP. Ketosis also enhances the production of important anti-oxidants that deal with toxic elements from our environments, including glutathione. Mitochondria from the hippocampus of ketogenic diet-fed animals are also resistant to mtDNA damage and are much less likely to commit cell suicide –apoptosis- at inappropriate times. As Douglas C. Wallace, PhD, Director of the Center for Mitochondrial and Epigenomic Medicine says, “the ketogenic diet may act at multiple levels: It may decrease excitatory neuronal activity, increase the expression of bioenergetic genes, increase mitochondrial biogenesis and oxidative energy production, and increase mitochondrial NADPH production, thus decreasing mitochondrial oxidative stress.”[21] Keto-adaptation results in marked changes in how we construct and maintain optimum membrane (“mem-brain”) composition, not only because of the healthy fats we provide through the diet, but also because of less free radical production and inflammatory mediators, along with more production of anti-oxidants. It is really the ideal balanced state. Moreover, you might want to keep in mind this excerpt from "Human Brain Evolution: The Influence of Freshwater and Marine Food Resources"[22]: There are two key advantages to having ketone bodies as the main alternative fuel to glucose for the human brain. First, humans normally have significant body fat stores, so there is an abundant supply of fatty acids to make ketones. Second, using ketones to meet part of the brain’s energy requirement when food availability is intermittent frees up some glucose for other uses and greatly reduces both the risk of detrimental muscle breakdown during glucose synthesis, as well as compromised function of other cells dependent on glucose, that is, red blood cells. One interesting attribute of ketone uptake by the brain is that it is four to five times faster in newborns and infants than in adults. Hence, in a sense, the efficient use of ketones by the infant brain means that it arguably has a better fuel reserve than the adult brain. Although the role of ketones as a fuel reserve is important, in infants, they are more than just a reserve brain fuel – they are also the main substrate for brain lipid synthesis. I have hypothesized that evolution of a greater capacity to make ketones coevolved with human brain expansion. This increasing capacity was directly linked to evolving fatty acid reserves in body fat stores during fetal and neonatal development. To both expand brain size and increase its sophistication so remarkably would have required a reliable and copious energy supply for a very long period of time, probably at least a million, if not two million, years. Initially, and up to a point, the energy needs of a somewhat larger hominin brain could be met by glucose and short – term glucose reserves such as glycogen and glucose synthesis from amino acids. As hominins slowly began to evolve larger brains after having acquired a more secure and abundant food supply, further brain expansion would have depended on evolving significant fat stores and having reliable and rapid access to the fuel in those fat stores. Fat stores were necessary but were still not sufficient without a coincident increase in the capacity for ketogenesis. This unique combination of outstanding fuel store in body fat as well as rapid and abundant availability of ketones as a brain fuel that could seamlessly replace glucose was the key fuel reserve for expanding the hominin brain, a reserve that was apparently not available to other land – based mammals, including nonhuman primates.It is indisputable that a ketogenic diet has protective effects in our brains. With all the evidence of its efficacy in mitochondrial dysfunction, it can be applied for all of us living in a highly stressful and toxic environment. Ketone bodies are healing bodies that helped us evolve and nowadays our mitochondria are always busted in some way or another since the odds in this toxic world are against us. Obviously, there are going to be people with such damaged mtDNA or with mutations they were born with, who can’t modify their systems (i.e. defects on L-carnitine metabolism), but even in some of those cases, they can halt or slow down further damage. Our healthy ancestors never had to deal with the levels of toxicity that we live nowadays and nevertheless, they ate optimally. Considering our current time and environment, the least we can do is eat optimally for our physiology. The way to have healing ketone bodies circulating in our blood stream is to do a high fat, restricted carb and moderated protein diet. Coupled with intermittent fasting which will enhance the production of ketone bodies, and resistance training which will create mitochondria with healthier mtDNA, we can beat the odds against us. What is considered nowadays a “normal diet” is actually an aberration based on the corruption of science which benefits Big Agra and Big Pharma. If we would go back in time to the days before the modern diet became normalized by corporative and agricultural interests, we will find that ketosis was the normal metabolic state. Today’s human metabolic state is aberrant. It is time to change that. References[1] A research member of sott.net’s forum has diabetes type 1 and is doing the ketogenic diet. Under normal circumstances, diabetics (including type I) report amazing results on a low-carbohydrate diet. See Dr. Bernstein’s Diabetics Solution by Richard K. Bernstein, MD (Little, Brown and Company: 2007). [2] It varies among each person, but the general range is between 0 and 70 grams of carbs plus moderate intake of protein, between 0.8 and 1.5 grams of protein per kg of ideal body weight. Pregnant women and children should not have their protein restricted. [3] Ketogenic diets in seizure control and neurologic disorders by Eric Kossoff, MD, Johns Hopkins Hospital, Baltimore, Maryland. The Art and Science of Low Carbohydrate Living by Jeff S. Volek, PhD, Rd and Stephen D. Phinney, MD, PhD. Beyond Obesity, LLC , 2011. [4] A Paoli, A Rubini, J S Volek and K A Grimaldi. Beyond weight loss: a review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets. European Journal of Clinical Nutrition (2013) 67, 789–796 [5] Rainer J Klement, Ulrike Kämmerer. Is there a role for carbohydrate restriction in the treatment and prevention of cancer? Nutr Metab (Lond). Oct 26, 2011; 8: 75. [6] If the genetic code is the hardware for life, the epigenetic code is software that determines how the hardware behaves. [7] David N. Ruskin and Susan A. Masino, The Nervous System and Metabolic Dysregulation: Emerging Evidence Converges on Ketogenic Diet Therapy. Front Neurosci. 2012; 6: 33. [8] Finkel T, Hwang PM. The Krebs cycle meets the cell cycle: mitochondria and the G1-S transition. Proc Natl Acad Sci U S A. 2009 Jul 21;106(29):11825-6. [9] Matthews C.M. Nurturing your divine feminine. Proc (Bayl Univ Med Cent). 2011 July; 24(3): 248. [10] Hipkiss AR. Energy metabolism, altered proteins, sirtuins and ageing: converging mechanisms? Biogerontology. 2008 Feb;9(1):49-55. [11] Saffran HA, Pare JM, Corcoran JA, et al. Herpes simplex virus eliminates host mitochondrial DNA. EMBO Rep. 2007 Feb;8(2):188-93. [12] Porcellini E, Carbone I, et al. Alzheimer’s disease gene signature says: beware of brain viral infections. Immun Ageing. 2010 Dec 14;7:16. [13] Gasior M, Rogawski MA, Hartman AL. Neuroprotective and disease-modifying effects of the ketogenic diet. Behav Pharmacol. 2006 Sep;17(5-6):431-9. [14] Maalouf M, Rho JM, Mattson MP. The neuroprotective properties of calorie restriction, the ketogenic diet, and ketone bodies. Brain Res Rev. 2009 Mar;59(2):293-315. [15] Nylen K, Velazquez JL. The effects of a ketogenic diet on ATP concentrations and the number of hippocampal mitochondria in Aldh5a1(-/-) mice. Biochim Biophys Acta. 2009 Mar;1790(3):208-12. [16] Bough K. Energy metabolism as part of the anticonvulsant mechanism of the ketogenic diet. Epilepsia. 2008 Nov;49 Suppl 8:91-3. [17] Finn PF, Dice JF. Ketone bodies stimulate chaperone-mediated autophagy. J Biol Chem. 2005 Jul 8;280(27):25864-70. [18] Yuk JM, Yoshimori T, Jo EK. Autophagy and bacterial infectious diseases. Exp Mol Med. 2012 Feb 29;44(2):99-108. [19] Chandra Wickramasinghe, Milton Wainwright & Jayant Narlika. SARS – a clue to its origins? The Lancet, vol. 361, May 23, 2003, pp 1832. [20] Yordy B, Iwasaki A. Autophagy in the control and pathogenesis of viral infection. Curr Opin Virol. 2011 Sep;1(3):196-203. [21] Douglas C. Wallace, Weiwei Fan, and Vincent Procaccio. Mitochondrial Energetics and Therapeutics Annu Rev Pathol. 2010; 5: 297–348. [22] Stephen Cunnane, Kathlyn Stewart.Human Brain Evolution: The Influence of Freshwater and Marine Food Resources. June 2010, Wiley-Blackwell. Gabriela Segura, MD Friday, 9 August 2013 Source: http://www.drmyhill.co.uk/wiki/Ketogenic_diet_-_a_connection_between_mitochondria_and_diet |



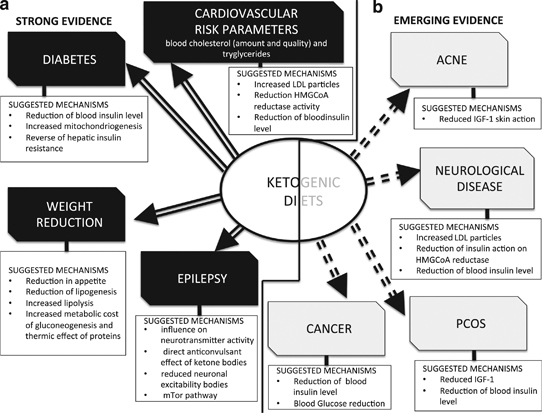
 RSS Feed
RSS Feed
